| Login | ||

Healthcare Training Institute - Quality Education since 1979
CE for Psychologist, Social Worker, Counselor, & MFT!!

Section 7
Defining Medical Error
Question 7 | Test | Table of Contents
The issue of patient safety plays a prominent role in health care. Its prominence is fueled by an expanding body of literature that shows a high incidence or error in medicine, [1–5] coupled with well-publicized medical error cases that have raised public concern about the safety of modern health care delivery.[6] As empirical literature on medical error expands, medicine’s vulnerability to error is becoming apparent. Medical errors are a leading cause of death in North America; [7] between 44 000 and 98 000 patients are estimated to die each year in the USA as a result of medical errors.[7]
To reduce the incidence of errors, health care providers must identify their causes, devise solutions and measure the success of improvement efforts. Moreover, accurate measurements of the incidence of error, based on clear and consistent definitions, are essential prerequisites for effective action.
Unfortunately and understandably, what is considered a medical error (if the term is used at all) has been influenced by differing contexts and purposes, such as research, quality control, ethics, insurance, legislation, legal action and statutory regulation.[1,3,5,10] As a result, a lack of standardized nomenclature and the use of multiple and overlapping definitions of medical error has hindered data synthesis and analysis, collaboration and evaluation of the impact of changes on health care delivery.[11–15]
Outcome-versus process dependent definitions
Historically, patient safety researchers investigating the impact of error in medicine have adopted outcome-dependant definitions of medical error and its surrogate terms, and have limited their focus to patients experiencing adverse outcomes or injury as a consequence of medical care. [1–5] Perhaps this tendency stems from a guiding principle of medical practice credited to Hippocrates, prium no nocere, which translates to "First, do no harm."[21, 25, 26] Moreover, the manner in which patient safety has been defined promotes an outcome-dependant approach to defining medical error.
Patient Safety: the avoidance, prevention and amelioration of adverse outcomes or injuries stemming from the process of healthcare (US National Patient Safety Foundation, 1999) [27]. Freedom from accidental injury (Institute of Medicine, 2000) [11].
In the earliest studies on patient safety in the 1950s, medical errors were largely considered "diseases of medical progress" [28] and dismissed as "the price we pay for modern diagnosis and therapy."[29] These reports tended to be limited to unusual patient reactions or those of magnitude and consequence. [28, 29]
In "Hazards of hospitalization," a pioneering investigation on error in medicine, Schimmel [18] maintained that "assessment of all untoward reactions, regardless of severity, is essential to determine their total incidence and to indicate the cumulative risk assumed by the patient exposed to the many drugs and procedures used in his care." With this imperative, he adopted the term noxious episode as a surrogate term for medical error, and studied prospectively the type and frequency of such episodes in patients admitted to a university medical service.
Noxious episode:all untoward events, complications, and mishaps that resulted from acceptable diagnostic or therapeutic measures deliberately instituted in the hospital (Schimmel, 1964).[18]
Reflecting the growing presence in the 1970s of third-party insurance companies in the economics of healthcare, The California Medical Insurance Feasibility Study [10] adopted the term potentially compensatable event to reflect errors that could potentially lead to malpractice claims.
Potentially compensatable event: an event due to medical management that resulted in disability, which led to or prolonged a hospitalization (The California Medical Insurance Feasibility Study, 1977). [10]
Adverse event: unintended injury to patients caused by medical management (rather than the underlying condition of the patient) that results in measurable disability, prolonged hospitalization or both (the Harvard Medical Practice Study, [1, 2] 1991, and the Utah and Colorado Medical Practice Study,[5] 1999).
Unintended injury or complication that results in disability, death, or prolonged hospital stay and is caused (including acts of omission and acts of commission) by health care management rather than the patients disease (Quality in Australian Health Study, 1995). [3, 4]
Although adverse events typically result from medical intervention, not all adverse patient outcomes are the result of error. Reflecting this fact, many investigators suggest that only preventable adverse events be attributed to medical error. [1,3,11,21,30] Patient safety experts have considered an adverse event to be preventable when
…there is a failure to follow accepted practice (the current level of expected performance for the average practitioner or system that manages the condition in question) at an individual or system level (Quality in Australian Health Study, 1995);[3] …it is widely established that a high incidence of this type of complication reflects low standards of care or technical expertise (Lucian Leape, 1994).[21]
Negligence: failure to meet the standard of care reasonably expected of an average physician qualified to take care of the patient in question (Brennan et al, 1991).[1] Care that fell below the standard expected of physicians in their community (Thomas et al, 1995).[5]
Negligent adverse event: injury caused by substandard medical management (Leape, 1991). [2]
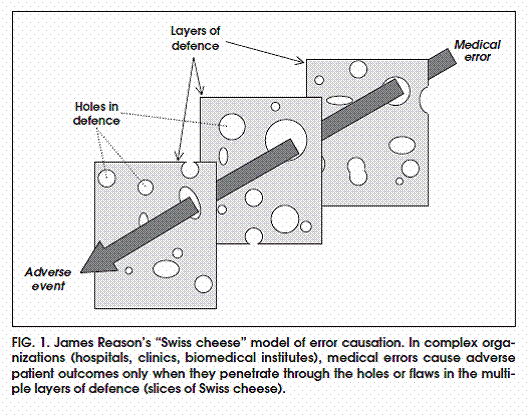
James Reason’s "Swiss cheese" model of error causation31 illustrates how this notion applies to health care (Fig. 1). According to Reason, most complex systems and work environments (such as hospitals) have several layers of defense that offer protection against the adverse consequences of error (signified by several slices of Swiss cheese).
In spite of such safeguards, several holes or flaws exist within each individual layer of defense (the holes in each individual slice). Injury to patients occurs only when circumstances arise that cause the flaws in each individual layer of protection (or holes in the cheese slices) to align in a way that allows an error to penetrate their defenses and reach the patient.[31]
A definition of medical error should capture process or system failures that cause errors, irrespective of outcome (a process-dependant approach). Ideally, process-dependant definitions of medical error should capture the full spectrum of medical errors, namely, errors that result in adverse patient outcomes as well as those that expose patients to risk but do not result in injury or harm. [11,16,33,34] Errors that do not result in injury are often referred to as near misses, close calls, potential adverse events or warning events.[34]
Near miss:any event that could have had an adverse patient consequence but did not, and was indistinguishable from a full-fledged adverse event in all but outcome (Barach and Small, 2000). [34]
Medical error: the failure of a planned action to be completed as intended (an error of execution) or the use of a wrong plan to achieve an aim (an error of planning) (Reason, 1990). [35] An unintended act (either of omission or commission) or one that does not achieve its intended outcome (Leape, 1994). [21] Deviations from the process of care, which may or may not cause harm to the patient (Reason, 2001). [14]
An outcome- and process- dependent definition of error
We propose the following definition:
Medical error: an act of omission or commission in planning or execution that contributes or could contribute to an unintended result.
This definition of medical error includes explicitly the key domains of error causation (omission and commission, planning and execution), and captures faulty processes that can and do lead to errors, whether adverse outcomes occur or not.
Medical, legal and governmental institutions must work collaboratively to break down the culture of blame while retaining methods for accountability. When this challenge has been met, health care institutions will no be constrained from measuring the most useful target for process improvement: all errors, whether or not they lead to adverse outcomes.
Conclusion
Medical errors represent an important public health problem and pose a serious threat to patient safety. The growing awareness of the frequency, causes and consequences of error in medicine reinforces an imperative to improve our understanding of the problem and to devise workable solutions and prevention strategies. Variations in nomenclature without a universally accepted definition of medical error hinder data collection and collaborative work to improve health care systems.
If health care providers and researchers are to improve patient safety, we must all speak the same language. The definition of medical error we have proposed explicitly addresses the key domains of error causation and includes process faults that have the potential for, but do not necessarily lead to, adverse patient outcomes.
--Grober, E. D., & Bohnen, J. A. (2005). Defining medical error. Canadian Journal Of Surgery, 48(1), 39-44.
Personal
Reflection Exercise #7
The preceding section contained information
about medical errors. Write one case study example
regarding how you might use the content of this section in your practice.
Reviewed 2023
Update
Root Cause Analysis and Medical Error Prevention
Singh, G., Patel, R. H., & Boster, J. (2023). Root Cause Analysis and Medical Error Prevention. In StatPearls. StatPearls Publishing.
Peer-Reviewed Journal Article References:
Garcia-Retamero, R., & Galesic, M. (2012). Doc, what would you do if you were me? On self–other discrepancies in medical decision making. Journal of Experimental Psychology: Applied, 18(1), 38–51.
Katz-Navon, T., Naveh, E., & Stern, Z. (2009). Active learning: When is more better? The case of resident physicians’ medical errors. Journal of Applied Psychology, 94(5), 1200–1209.
McKay, D., & Jensen-Doss, A. (2021). Harmful treatments in psychotherapy. Clinical Psychology: Science and Practice, 28(1), 2-4.
Reader, T. W., & Gillespie, A. (2021). Stakeholders in safety: Patient reports on unsafe clinical behaviors distinguish hospital mortality rates. Journal of Applied Psychology, 106(3), 439–451.
Robiner, W. N., Tompkins, T. L., & Hathaway, K. M. (2020). Prescriptive authority: Psychologists’ abridged training relative to other professions’ training. Clinical Psychology: Science and Practice, 27(1), Article e12309
QUESTION 7
What is patient safety? To select and enter your answer go to Test.
Test
Section 8
Table of Contents
Top
Excerpts from Bibliography referenced in this article
1. Brennan TA, Leape LL, Laird NM, Hebert L, Localio AR, Lawthers AG, et al. Incidence of adverse events and negligence in hospitalized patients: results of the Harvard Medical Practice Study I. N Engl J Med 1991;324:370-6.
2. Leape LL, Brennan TA, Laird N, Lawthers AG, Localio AR, Barnes BA, et al. The nature of adverse events in hospitalized patients: results of the Harvard Medical Practice Study II. N Engl J Med 1991; 324:377-84.
3. Wilson RM, Runciman WB, Gibberd RW, Harrison BT, Newby L, Hamilton JD. The Quality in Australian Health Care Study. Med J Aust 1995;163:458-71.
4. Wilson RM, Harrison GB, Gibberd RW, Hamilton JD. An analysis of the causes of adverse events from the Quality in Australian Health Care Study. Med J Aust 1999;170:411-5.
5. Thomas EJ, Studdert DM, Burstin HR, Orav EJ, Zeena T, Williams EJ, et al. Incidence and types of adverse events and negligent care in Utah and Colorado. Medical Care 1999;38(3):261-71.
6. Cook R, Woods D, Miller C. A tale of two stories: contrasting views of patient safety. Chicago: National Patient Safety Foundation; 1998.
7. American Hospital Association. Hospital statistics. Chicago: the Association; 1999.
10. Mills DH, Boyden JS, Rubamen DS. Report on The Medical Insurance Feasibility Study. San Francisco (CA): Sutter Publications; 1977.
11. Kohn LT, Corrigan JM, Donaldson MS. To err is human: building a safer health system. Washington: National Academy Press; 2000.
12. Hebert PC, Levin AV, Robertson G. Bioethics for clinicians 23: disclosure of medical error. CMAJ 2001;164(4):509-13.
13. Hatch D. Incidence and acceptance of errors in medicine. Schweiz Arzte, Bull Med Swiss 2001;82:1339-43.
14. Reason JT. Understanding adverse events: the human factor. In: Vincent C, editor. Clinical risk management: enhancing patient safety. London: BMJ Publishing Group; 2001. p. 9-30.
15. Senders JW. Medical devices, medical errors and medical accidents. In: Bogner MS, editor. Human error in medicine. Hillsdale (NJ): Lawrence Erlbaum Associates; 1994.
18. Schimmel EM. The hazards of hospitalization. Ann Intern Med 1964;60:100-9.
21. Leape L. Error in medicine. JAMA 1994; 272:1851-7.
25. Veatch RM. Cross cultural perspectives in medical ethics readings. Boston: Jones and Bartlett Publishers; 1989.
26. Nightingale F. Notes on hospitals. London: Longman; 1863.
27. National Patient Safety Foundation. Agenda for research and development in patient safety. Available: www.npsf.org (accessed 2005 Jan 14).
28. Moser RH. Diseases of medical progress.
N Engl J Med 1956;255:606-14.
29. Barr DP. Hazards of modern diagnosis and therapy: the price we pay. JAMA 1955;159:1452-6.
30. Nora PF. Improving safety for surgical patients: suggested strategies. Bull Am Coll Surg 2000;85(9):11-4.
31. Reason J. Managing the risks of organizational accidents. Aldershot: Ashgate; 1997.
33. Holloway RG, Panzer RJ. Lawyers, litigation, and liability: Can they make patients safer? Neurology 2001;56(8):24-5.
34. Barach P, Small SD. Reporting and preventing medical mishaps: lessons form non-medical near miss reporting. BMJ 2000;320:759-63.

